Nipah virus (NiV) – Introduction, Morphology, Pathogenicity, Lab Diagnosis, Treatment, Prevention, and Keynotes
Introduction
Nipah virus (NiV) is a highly contagious and deadly zoonotic virus that belongs to the family Paramyxoviridae, genus Henipavirus. It was first identified in 1999 during an outbreak in Malaysia, which affected both humans and pigs. Nipah virus is known for causing severe respiratory and neurological diseases in humans, and it has the potential for human-to-human transmission.
Here is an introduction to Nipah virus:
1. Origin: Nipah virus is believed to originate from fruit bats (Pteropus spp.), which serve as natural reservoirs for the virus. These bats do not typically show signs of illness when infected with NiV.
2. Transmission: The primary mode of transmission to humans is through direct contact with infected animals, consumption of contaminated food or fruits, or exposure to bodily fluids of infected animals. Human-to-human transmission has occurred, primarily through close contact with infected individuals.
3. Clinical Presentation: Nipah virus infection can lead to a range of clinical symptoms, including fever, headache, drowsiness, and confusion. It can progress to severe respiratory distress and encephalitis, which can be fatal. The virus has a high mortality rate, with death occurring in a significant proportion of cases.
4. Outbreaks: Nipah virus outbreaks have occurred primarily in South and Southeast Asia, including Malaysia, Singapore, Bangladesh, and India. These outbreaks often involve close contact with infected pigs and consumption of raw date palm sap contaminated with bat saliva or urine.
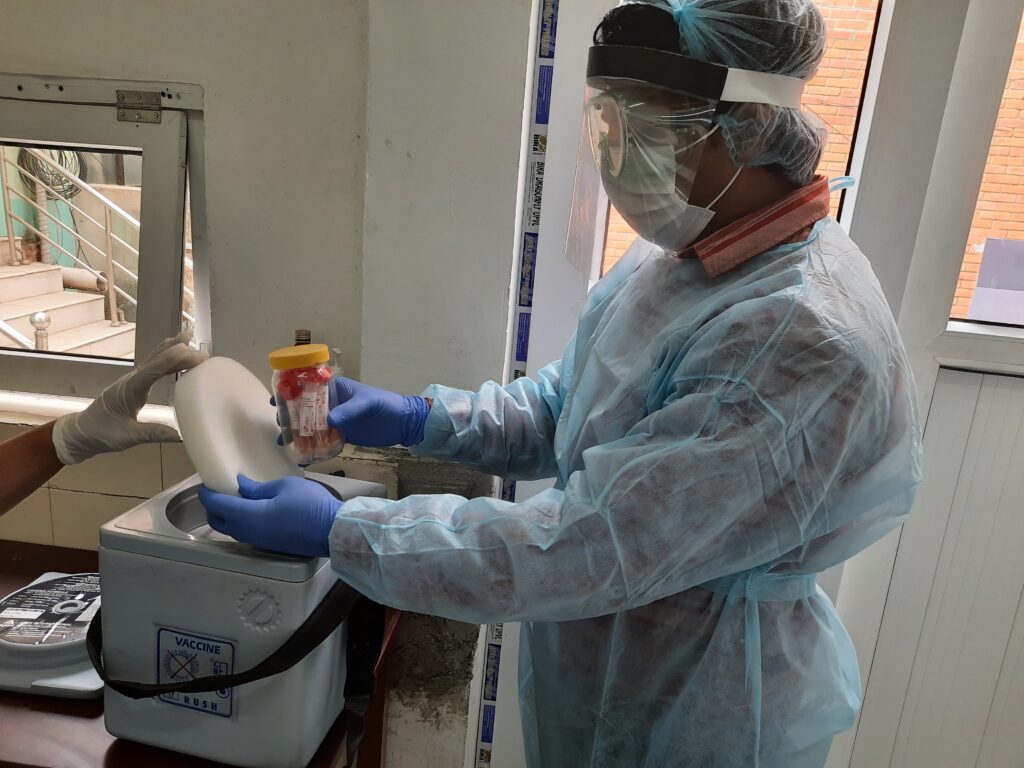
5. Diagnosis: Laboratory tests, including polymerase chain reaction (PCR) and serological tests, are used to confirm Nipah virus infection. Samples of blood, cerebrospinal fluid, throat swabs, or urine are collected for testing.
6. Treatment: There is no specific antiviral treatment for Nipah virus infection. Supportive care, including mechanical ventilation and intensive medical management, is provided to relieve symptoms and improve the patient’s chances of survival.
7. Prevention: Preventing Nipah virus infection involves various measures, including avoiding direct contact with infected animals, refraining from consuming raw date palm sap, implementing strict infection control practices in healthcare settings, and conducting public health awareness campaigns in affected regions.
8. Vaccine Development: Research is ongoing to develop vaccines against Nipah virus. Several experimental vaccines have shown promise in preclinical studies and may offer a means of preventing future outbreaks.
9. Global Concern: Nipah virus is considered a global health threat due to its high mortality rate, potential for human-to-human transmission, and lack of specific antiviral treatments. It is classified as a Biosafety Level 4 (BSL-4) pathogen, indicating its high level of infectiousness and potential for severe disease.
Morphology
Nipah virus (NiV) is a negative-sense, single-stranded RNA virus that belongs to the Paramyxoviridae family, genus Henipavirus. While viruses like NiV do not have the traditional cellular structures of bacteria or eukaryotic cells, they do have a specific morphology when viewed at the microscopic level. Here are some key characteristics of NiV’s morphology:
- Viral Particle (Virion) Size: Nipah virus is relatively large compared to some other viruses. It typically ranges in size from approximately 40 to 60 nanometers (nm) in diameter. This size can vary slightly depending on the virus strain and how it is prepared for imaging.
- Shape: Nipah virus particles have a pleomorphic (variable shape) appearance. They can be elongated or filamentous in shape, but they are often described as having a roughly spherical or ovoid shape with a lipid envelope.
- Envelope: Like many other viruses, NiV is enveloped, which means it is surrounded by a lipid bilayer membrane derived from the host cell. This envelope contains viral glycoproteins that are critical for attachment to and entry into host cells.
- Surface Glycoproteins: Nipah virus has two major surface glycoproteins, often referred to as the G and F proteins. These glycoproteins play a crucial role in the virus’s ability to bind to host cell receptors and facilitate membrane fusion during viral entry.
- Helical Nucleocapsid: Inside the viral envelope is a helical nucleocapsid structure composed of the viral RNA genome complexed with nucleocapsid (N) protein. This helical nucleocapsid is a characteristic feature of negative-sense RNA viruses like NiV.
- Heterogeneity: It’s important to note that NiV particles can exhibit some degree of heterogeneity in their morphology. This variability in size and shape is observed in electron microscopy and is common among enveloped viruses.
Nipah virus’s pleomorphic envelope and surface glycoproteins are essential for its interactions with host cells, allowing it to enter and infect the host. These structural features are critical for understanding the virus’s pathogenesis and for developing potential therapeutic interventions.
Pathogenicity
The pathogenicity of Nipah virus (NiV) is characterized by its ability to cause severe and often fatal diseases in both animals and humans. NiV is considered a highly pathogenic zoonotic virus, meaning it can be transmitted from animals to humans and cause severe disease. Here are key aspects of NiV’s pathogenicity:
- Severe Clinical Presentation: Nipah virus infection in humans can lead to a range of clinical symptoms, including fever, headache, cough, and respiratory distress. However, what distinguishes NiV is its propensity to cause severe encephalitis (inflammation of the brain), which often leads to coma and death. Other neurological symptoms can include confusion, disorientation, and seizures.
- Respiratory and Neurological Involvement: NiV can affect multiple organ systems, with the respiratory and neurological systems being the most severely impacted. Respiratory symptoms can progress rapidly to acute respiratory distress syndrome (ARDS), a life-threatening condition.
- High Mortality Rate: Nipah virus infection has a high mortality rate, often exceeding 70% in outbreaks. The death rate can vary depending on factors such as the virus strain, the quality of medical care, and the timing of treatment.
- Human-to-Human Transmission: While NiV is primarily transmitted to humans from infected animals (particularly fruit bats) or through the consumption of contaminated food or fruits, human-to-human transmission has been documented, especially in healthcare settings. This is a significant concern because it can lead to larger outbreaks.
- Host Range: NiV can infect a wide range of animals, including pigs, dogs, cats, and various wildlife species. Pigs are considered amplifying hosts, and outbreaks often involve these animals. Intermediate hosts, such as horses, have also been implicated in transmission.
- Cellular Entry Mechanism: NiV has a unique cellular entry mechanism mediated by its surface glycoproteins, particularly the G (attachment) and F (fusion) proteins. These glycoproteins enable the virus to bind to host cell receptors, initiate membrane fusion, and enter host cells efficiently.
- Immune Evasion: NiV has evolved various strategies to evade the host immune response, including inhibiting interferon production and countering the host’s antiviral defenses. This contributes to the virus’s ability to establish a systemic infection.
- Potential for Spillover: Nipah virus spillover events, where the virus crosses over from animals to humans, are a recurring concern, particularly in regions where bats are the natural reservoir. Changes in land use, agriculture, and urbanization can increase the risk of spillover events.
- Public Health Impact: Nipah virus outbreaks have a significant impact on public health systems, often requiring intensive efforts for contact tracing, isolation of cases, and infection control measures in healthcare settings.
Lab Diagnosis
The laboratory diagnosis of Nipah virus (NiV) infection is a critical step in identifying and confirming cases, especially during outbreaks. Prompt and accurate diagnosis helps in implementing appropriate public health measures and clinical management. Here are the key laboratory methods and tests used for diagnosing NiV:
- Clinical Evaluation: Clinical assessment of patients with suspected NiV infection is the initial step in diagnosis. Healthcare providers should consider symptoms such as fever, encephalitis, and respiratory distress, as well as relevant exposure history (e.g., contact with bats or sick animals).
- Collection of Clinical Samples: Samples from suspected NiV cases should be collected under strict biosafety measures to minimize the risk of laboratory-acquired infections. The following types of clinical samples can be collected:
- Blood: Serum and plasma samples are commonly used for serological tests.
- Respiratory Secretions: Throat and nasal swabs may be collected for PCR testing.
- Cerebrospinal Fluid (CSF): If neurological symptoms are present, CSF may be tested for viral RNA.
- Tissues: In fatal cases, post-mortem tissue samples may be collected for diagnostic purposes.
- Serological Tests:
- Enzyme-Linked Immunosorbent Assay (ELISA): ELISA tests detect NiV-specific antibodies (IgM and IgG) in serum samples. A rising IgG titer over time can indicate recent infection.
- Molecular Tests:
- Polymerase Chain Reaction (PCR): PCR tests can detect NiV RNA in clinical samples. Reverse transcription polymerase chain reaction (RT-PCR) is commonly used to amplify viral RNA.
- Virus Isolation:
- Cell Culture: NiV can be isolated from clinical samples using cell culture techniques, but this method requires a high-level biosafety containment facility (BSL-4).
- Immunohistochemistry (IHC): In post-mortem cases, IHC can be used to detect NiV antigens in tissue samples.
- Next-Generation Sequencing (NGS): NGS techniques can be employed for genomic sequencing and phylogenetic analysis to identify the NiV strain and its genetic characteristics.
- Antigen Detection: While less commonly used, NiV antigens can be detected in clinical samples using specific antibodies in diagnostic assays.
It’s essential to note that NiV diagnosis should be performed in specialized laboratories with the appropriate biosafety precautions, as the virus is classified as a Biosafety Level 4 (BSL-4) pathogen. Additionally, clinical and epidemiological information, including exposure history and travel history, should be considered in conjunction with laboratory results to confirm a NiV infection.
Because NiV infections can progress rapidly and have a high mortality rate, early diagnosis and appropriate patient management are crucial. Suspected cases should be isolated, and infection control measures should be implemented to prevent further transmission, especially in healthcare settings.
Treatment
Management of NiV infection primarily involves supportive care to alleviate symptoms and complications. Here are the key aspects of NiV treatment:
- Isolation and Infection Control: Suspected or confirmed cases of NiV infection should be isolated to prevent further transmission. Strict infection control measures should be implemented, especially in healthcare settings, to minimize the risk of nosocomial (hospital-acquired) infections.
- Supportive Care: Supportive care is the cornerstone of NiV treatment. This includes:
- Respiratory Support: Patients with respiratory distress may require mechanical ventilation or oxygen therapy.
- Fluid and Electrolyte Balance: Maintaining proper hydration and managing electrolyte imbalances is crucial.
- Fever Management: Fever-reducing medications may be administered to control high body temperatures.
- Antipyretics and Analgesics: Medications such as acetaminophen (paracetamol) can be used to reduce fever and relieve pain.
- Anticonvulsants: In cases where patients develop seizures or other neurological symptoms, anticonvulsant medications may be administered.
- Antibiotics: Initially, broad-spectrum antibiotics may be prescribed until bacterial infections are ruled out. NiV itself is a viral infection and does not respond to antibiotics.
- Experimental Treatments: During outbreaks, experimental treatments and therapies may be considered, including antiviral drugs that have shown promise in preclinical studies. However, the effectiveness and safety of these treatments are still being studied, and they are not widely available.
- Potential for Passive Immunotherapy: Passive immunotherapy, such as monoclonal antibodies or convalescent plasma from recovered patients, has been explored as a potential treatment option for NiV. These therapies aim to provide the patient with antibodies against the virus.
- Research and Clinical Trials: Ongoing research efforts are focused on developing specific antiviral drugs and vaccines for NiV. Clinical trials may be conducted to assess the safety and efficacy of these treatments.
It’s important to note that NiV infection carries a high mortality rate, and the availability of specific treatments is limited. Prevention measures, including public health interventions to control outbreaks and reduce the risk of spillover from animals to humans, are crucial in managing NiV.
Prevention
Preventing Nipah virus (NiV) infection is crucial, particularly in regions where outbreaks have occurred. NiV is a zoonotic virus, meaning it can be transmitted from animals to humans. Implementing preventive measures can help reduce the risk of NiV transmission and protect individuals and communities. Here are key strategies for preventing NiV infection:
- Avoid Close Contact with Infected Animals:
- Do not handle or consume animals that appear sick or have died from unknown causes.
- Avoid direct contact with bats, particularly fruit bats, as they are considered the natural reservoir of NiV.
- Practice Good Hygiene:
- Wash hands thoroughly with soap and water after handling animals or animal products.
- Avoid consuming raw date palm sap, especially if it has been collected in open containers that may be contaminated by bats.
- Food Safety Measures:
- Ensure that fruits and vegetables are thoroughly washed and cleaned before consumption.
- Avoid consumption of fruits or palm sap with visible signs of contamination.
- Proper Cooking and Food Handling:
- Cook meat and animal products thoroughly to kill potential pathogens.
- Practice safe food handling and storage to prevent cross-contamination.
- Use of Personal Protective Equipment (PPE):
- If working in environments with a high risk of NiV exposure (e.g., healthcare settings), healthcare workers should use appropriate PPE to prevent contact with bodily fluids.
- Infection Control Measures in Healthcare Settings:
- Implement strict infection control measures in healthcare facilities, including isolation of suspected cases, use of PPE, and adherence to proper hand hygiene practices.
- Hospitalized patients with suspected NiV infection should be isolated, and healthcare workers should follow strict infection prevention protocols.
- Quarantine and Surveillance:
- Monitor and quarantine individuals who have had close contact with confirmed or suspected NiV cases to prevent further transmission.
- Conduct surveillance in regions where NiV outbreaks have occurred to identify and respond to cases promptly.
- Public Health Awareness and Education:
- Conduct public health awareness campaigns to educate communities about NiV transmission risks and prevention measures.
- Encourage communities to report any sick animals or unusual deaths to local authorities.
- Avoiding Unnecessary Movement during Outbreaks:
- During NiV outbreaks, avoid unnecessary travel to affected areas to reduce the risk of exposure.
- Research and Vaccine Development:
- Support research efforts to develop vaccines and antiviral treatments for NiV.
- Monitoring and Reporting:
- Establish surveillance systems to monitor for NiV outbreaks and promptly report suspected cases to health authorities.
- Environmental Measures:
- Implement measures to deter bats from roosting in or near human habitats, especially in agricultural areas.
Keynotes
Here are keynotes summarizing important information about Nipah virus (NiV):
- Classification: Nipah virus (NiV) is a zoonotic virus belonging to the Paramyxoviridae family, Henipavirus genus. It was first identified in Malaysia in 1999.
- Natural Reservoir: Fruit bats (Pteropus spp.), also known as flying foxes, are considered the natural reservoir of NiV. These bats are asymptomatic carriers of the virus.
- Transmission: NiV is primarily transmitted from bats to humans through direct contact with infected bats, consumption of contaminated food or fruits, or exposure to bodily fluids of infected animals. Human-to-human transmission has occurred, mainly in healthcare settings.
- Clinical Presentation: NiV infection in humans can lead to a range of clinical symptoms, including fever, headache, respiratory distress, and encephalitis. Severe cases can result in coma and a high mortality rate.
- Outbreaks: Nipah virus outbreaks have occurred in several countries in South and Southeast Asia, including Malaysia, Singapore, Bangladesh, and India. Pigs have been implicated as intermediate hosts in some outbreaks.
- Laboratory Diagnosis: Laboratory diagnosis involves serological tests (ELISA), molecular tests (PCR), and virus isolation from clinical samples. Diagnosis should be performed in specialized biosafety containment facilities due to the virus’s high pathogenicity.
- Treatment: There is no specific antiviral treatment for NiV infection. Supportive care is provided to manage symptoms, and experimental treatments and therapies are being researched.
- Prevention: Prevention measures include avoiding close contact with infected animals, practicing good hygiene, safe food handling, and proper cooking. In healthcare settings, infection control measures are crucial.
- Vaccine Development: Research is ongoing to develop vaccines against NiV. Several experimental vaccines have shown promise in preclinical studies.
- Public Health Concern: NiV is considered a public health threat due to its high mortality rate, potential for human-to-human transmission, and lack of specific treatment or vaccine. It is classified as a Biosafety Level 4 (BSL-4) pathogen.
- Community Education: Public health awareness campaigns and community engagement are essential to educate people about NiV transmission risks and preventive measures.
- One Health Approach: NiV prevention and control efforts often require collaboration between human health, animal health, and environmental health sectors due to its zoonotic nature.
Further Readings
- Scientific Journals:
- Look for research articles, reviews, and case reports related to Nipah virus in scientific journals. Key journals include:
- Emerging Infectious Diseases
- The Lancet Infectious Diseases
- PLOS Neglected Tropical Diseases
- Virology Journal
- Look for research articles, reviews, and case reports related to Nipah virus in scientific journals. Key journals include:
- Books:
- Textbooks on virology, infectious diseases, and epidemiology may have chapters dedicated to Nipah virus. Examples include “Principles of Virology” by Flint et al. and “Control of Communicable Diseases Manual” by Heymann.
- Government Health Agencies:
- Visit the websites of health organizations like the World Health Organization (WHO), the Centers for Disease Control and Prevention (CDC), and the National Institutes of Health (NIH) for comprehensive information, reports, and guidelines on Nipah virus.
- Academic Institutions:
- University websites and academic institutions specializing in infectious diseases often publish research findings, reports, and educational resources related to Nipah virus.
- Research Centers:
- Research centers and institutes focused on emerging infectious diseases and virology, such as the CDC’s Viral Special Pathogens Branch, may have in-depth information on Nipah virus research.
- Government Reports:
- Look for government reports and publications related to Nipah virus outbreaks and control efforts, especially in affected countries.
- International Health Organizations:
- The World Health Organization (WHO) often publishes situation reports, guidelines, and research findings related to Nipah virus.
- Online Databases:
- Utilize online databases like PubMed, Google Scholar, and Web of Science to search for specific research papers and articles related to Nipah virus.
- Conference Proceedings:
- Explore conference proceedings from virology and infectious disease conferences, as they may include recent research findings and updates on Nipah virus.
- Medical and Scientific News Sources:
- Stay updated on the latest developments and research through reputable medical and scientific news outlets.
