Coccidian Parasites-Introduction, Morphology, Pathogenicity, Lab Diagnosis, Treatment, Prevention, and Keynotes
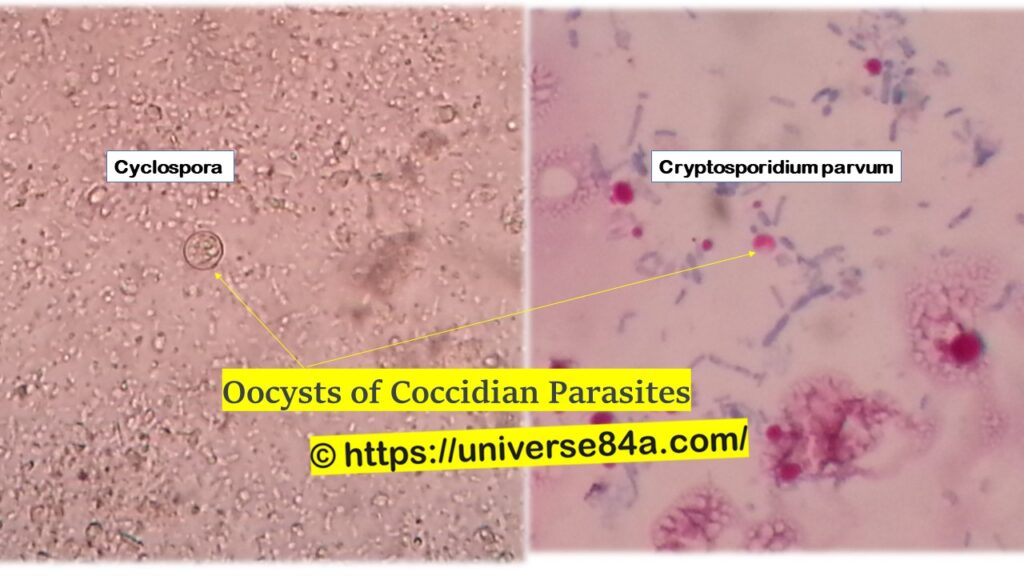
Introduction
Coccidian parasites are a diverse group of protozoan parasites that belong to the phylum Apicomplexa. They are named after their characteristic intracellular form called the coccidian, which is a spore-like structure. These parasites have a complex life cycle, typically involving both sexual and asexual stages, and they infect the gastrointestinal tract of a wide range of animals, including humans.
The most well-known genera of coccidian parasites include Cryptosporidium, Cyclospora, and Toxoplasma. These parasites have different species that can cause diseases in their respective hosts, leading to a variety of clinical manifestations. In humans, coccidian infections can result in gastrointestinal symptoms such as diarrhea, abdominal pain, and vomiting.
Coccidian parasites are transmitted through the ingestion of infective stages, such as oocysts, which are shed in the feces of infected hosts. The oocysts can contaminate water, soil, or food sources, and when ingested by a susceptible host, they initiate the infection cycle. Certain coccidian parasites, such as Toxoplasma gondii, can also be transmitted through other routes, such as ingestion of undercooked meat or vertical transmission from an infected mother to her fetus.
Morphology
Coccidian parasites exhibit a characteristic morphology that is common among the members of the phylum Apicomplexa. However, there may be some variations in the morphology of different genera and species within the coccidian group. Here is a general overview of the morphology of coccidian parasites:
- Oocysts: The oocyst is the infective stage of coccidian parasites. It is a spore-like structure that is produced within the host’s gastrointestinal tract. Oocysts are usually composed of a thick, resistant outer wall that protects the internal contents. The size and shape of oocysts can vary between different coccidian species, ranging from spherical to ellipsoidal or ovoid shapes. They are often observed in fecal samples during the diagnosis of coccidian infections.
- Sporozoites: Inside the oocyst, sporozoites are the infective forms that are released when the oocyst is ingested by a susceptible host. Sporozoites are elongated, motile structures that possess specialized organelles, such as apical complex and micronemes, which aid in their attachment and invasion of host cells.
- Trophozoites: Once inside the host’s cells, the sporozoites transform into trophozoites. Trophozoites are the active, growing stage of coccidian parasites. They are characterized by their unique apical complex, which contains specialized organelles, including micronemes and rhoptries, involved in host cell invasion and nutrient uptake.
- Schizonts: Trophozoites undergo a series of asexual divisions known as schizogony or merogony, resulting in the formation of schizonts. Schizonts are multinucleated structures that contain numerous daughter cells called merozoites.
- Merozoites: Merozoites are the infective forms that are released from schizonts. They are small, typically elongated structures that are capable of invading new host cells and initiating the next cycle of infection. Merozoites may possess specialized structures, such as apical organelles and rhoptries, for host cell penetration.
- Gametocytes: Under certain conditions, some coccidian parasites undergo sexual reproduction. Gametocytes are the sexual stages of coccidian parasites, and they develop within host cells. Male and female gametocytes fuse to form zygotes, which then develop into oocysts, completing the life cycle of coccidian parasites.
Pathogenicity
Coccidian parasites can exhibit varying degrees of pathogenicity depending on the species, the host’s immune status, and other factors. While some coccidian parasites may cause mild or self-limiting infections, others can lead to severe or even life-threatening diseases. Here are some examples of pathogenic coccidian parasites and the diseases they cause:
- Cryptosporidium spp.: Cryptosporidium parasites, particularly Cryptosporidium hominis and Cryptosporidium parvum, are known to cause cryptosporidiosis in humans. This parasitic infection primarily affects the gastrointestinal tract, leading to symptoms such as watery diarrhea, abdominal cramps, nausea, and vomiting. Cryptosporidiosis can be particularly severe and prolonged in immunocompromised individuals, such as those with HIV/AIDS.
- Cyclospora cayetanensis: Cyclospora cayetanensis is responsible for causing cyclosporiasis, a gastrointestinal illness characterized by watery diarrhea, abdominal cramps, bloating, and fatigue. Cyclosporiasis is usually self-limiting but can be prolonged and debilitating in some cases, especially in individuals with weakened immune systems.
- Toxoplasma gondii: Toxoplasma gondii is a widely distributed coccidian parasite that can infect humans and various warm-blooded animals. In most healthy individuals, the infection may be asymptomatic or result in mild flu-like symptoms. However, in immunocompromised individuals, such as those with HIV/AIDS or organ transplant recipients, Toxoplasma infection can cause severe toxoplasmosis, affecting multiple organs, including the brain, eyes, and lungs. In pregnant women, Toxoplasma infection can lead to congenital toxoplasmosis, which can result in miscarriage, stillbirth, or long-term health problems in the newborn.
- Isospora belli: Isospora belli is a coccidian parasite that causes isosporiasis in humans. It primarily affects the gastrointestinal tract, leading to symptoms such as watery diarrhea, abdominal cramps, and weight loss. Isosporiasis is more commonly observed in individuals with compromised immune systems, such as those with HIV/AIDS.
- Sarcocystis spp.: Sarcocystis species are coccidian parasites that infect a variety of animals, including humans. Human infections are usually acquired through consumption of undercooked meat containing cysts of Sarcocystis parasites. In most cases, sarcocystosis is asymptomatic or causes mild gastrointestinal symptoms. However, in rare instances, severe infections with Sarcocystis can lead to muscle pain, fatigue, and neurological manifestations.
Lab Diagnosis
The laboratory diagnosis of coccidian parasites typically involves the detection and identification of the parasite stages or their genetic material in clinical samples. Here are some common methods used for the laboratory diagnosis of coccidian parasites:
- Microscopic Examination: Microscopic examination of clinical samples, such as feces or tissue samples, is a commonly used method for diagnosing coccidian infections. This involves preparing a smear or a concentrated sample and examining it under a microscope. Specific staining techniques, such as acid-fast staining (e.g., modified Ziehl-Neelsen stain) or fluorescent staining (e.g., auramine-rhodamine stain), may be employed to enhance the visualization of coccidian parasites. The characteristic morphology of oocysts, sporozoites, trophozoites, and other stages can help identify the species of coccidian parasites.
- Molecular Techniques: Molecular methods, such as polymerase chain reaction (PCR), are increasingly being used for the detection and identification of coccidian parasites. PCR can amplify specific genetic regions of the parasite’s DNA, allowing for the accurate identification of the species. It is a sensitive and specific method and can be particularly useful when the parasite load is low or in cases where microscopic examination alone may not be sufficient.
- Immunological Tests: Immunological assays, such as enzyme-linked immunosorbent assays (ELISAs), can be used to detect specific antibodies or antigen components of coccidian parasites in blood samples. These tests can help determine if a person has been exposed to or is currently infected with a particular coccidian parasite. They are commonly used for diagnosing infections caused by parasites like Cryptosporidium and Toxoplasma.
- Histopathological Examination: In cases where coccidian parasites have invaded tissues, histopathological examination of biopsy samples can be performed. Tissue sections are stained using specialized techniques, such as hematoxylin and eosin (H&E) staining, to visualize the parasites within the host tissues. Histopathological examination can provide valuable information about the site and extent of tissue damage caused by coccidian parasites.
- Serological Tests: Serological tests, such as indirect fluorescent antibody (IFA) tests or Western blot assays, are used to detect specific antibodies against coccidian parasites in a person’s blood. These tests can help determine previous exposure or current infection. Serological tests are commonly employed for diagnosing infections caused by parasites like Toxoplasma.
It’s important to note that the choice of diagnostic method depends on several factors, including the type of coccidian parasite suspected, the clinical presentation, the availability of laboratory resources, and the expertise of the laboratory personnel. It is recommended to consult a healthcare professional or a laboratory specialist for appropriate testing and interpretation of the results.
Treatment
The treatment of coccidian parasites depends on the specific parasite species causing the infection and the severity of the disease. Antiparasitic medications are commonly used to target and eliminate coccidian parasites. Here are some examples of medications used in the treatment of coccidian infections:
- Nitazoxanide: Nitazoxanide is a broad-spectrum antiparasitic medication that is effective against several coccidian parasites, including Cryptosporidium parvum and Cryptosporidium hominis. It is commonly used for the treatment of cryptosporidiosis in both children and adults. Nitazoxanide works by inhibiting the energy metabolism of the parasites and disrupting their cellular function.
- Sulfonamides: Sulfonamide medications, such as sulfadiazine and sulfamethoxazole, are commonly used for the treatment of coccidian infections, including toxoplasmosis. These drugs work by inhibiting the synthesis of folate, a vital nutrient for the parasites. Sulfonamides are often used in combination with other medications, such as pyrimethamine, for a more effective treatment.
- Pyrimethamine: Pyrimethamine is an antiparasitic medication that is frequently used in combination with sulfonamides for the treatment of toxoplasmosis. It works by inhibiting the parasite’s ability to utilize folic acid. This combination therapy is often used for immunocompromised individuals, such as those with HIV/AIDS, to prevent severe toxoplasmosis.
- Atovaquone: Atovaquone, along with proguanil, is commonly used for the treatment and prevention of malaria. It also has some efficacy against certain coccidian parasites, such as Cryptosporidium parvum. Atovaquone inhibits the parasite’s ability to generate energy by targeting the electron transport chain within the parasite’s mitochondria.
- Clindamycin: Clindamycin is an antibiotic that has some activity against certain coccidian parasites, including Toxoplasma gondii. It inhibits protein synthesis within the parasites, leading to their death. Clindamycin is often used in combination with other medications, such as sulfadiazine, for the treatment of severe toxoplasmosis.
- It is important to note that the choice of medication and the duration of treatment may vary depending on the specific coccidian parasite, the severity of the infection, and the individual’s immune status. Treatment should be guided by a healthcare professional who can consider the individual’s overall health, potential drug interactions, and any underlying conditions. Additionally, supportive measures, such as rehydration and management of symptoms, may be necessary to ensure the patient’s comfort and recovery.
Prevention
Preventing coccidian parasite infections involves implementing measures to minimize exposure to the parasites and interrupt their transmission. Here are some key prevention strategies:
- Practice Good Hygiene: Proper hygiene practices are crucial in preventing coccidian infections. This includes regular handwashing with soap and water, especially before eating or preparing food, after using the toilet, and after contact with animals or potentially contaminated environments. Hand sanitizers can be used when soap and water are not available.
- Ensure Safe Food and Water: Coccidian parasites can be transmitted through contaminated food and water sources. To reduce the risk of infection, it is important to:
- Wash fruits and vegetables thoroughly before consumption.
- Avoid consuming raw or undercooked meat, especially from unknown or unreliable sources.
- Drink safe and clean water. If the water source is questionable, consider using bottled water or water that has been properly treated and filtered.
- Practice Safe Animal Handling: Some coccidian parasites, such as Toxoplasma gondii, can be transmitted through contact with infected animals or their feces. To minimize the risk:
- Wear gloves when handling soil, sand, or potentially contaminated materials.
- Wash hands thoroughly after handling animals, particularly cats, and their litter boxes.
- Avoid direct contact with stray or wild animals.
- Pregnant women should avoid cleaning litter boxes to reduce the risk of toxoplasmosis.
- Maintain Clean Living Environments: Proper sanitation and cleanliness in living environments are essential in preventing coccidian infections. This includes:
- Cleaning and disinfecting surfaces that may come into contact with feces or contaminated materials.
- Regularly cleaning and disinfecting animal enclosures, litter boxes, and other pet-related areas.
- Avoiding overcrowding and maintaining good hygiene practices in animal husbandry settings, such as farms and breeding facilities.
- Implement Food Safety Practices: In food handling and preparation, following food safety guidelines is crucial. This includes:
- Properly cooking meat to recommended temperatures to kill any potential parasites.
- Avoiding cross-contamination by using separate cutting boards, utensils, and plates for raw and cooked foods.
- Refrigerating perishable foods promptly and ensuring proper storage temperatures.
- Be Mindful of Environmental Contamination: Coccidian parasites can persist in the environment, such as soil and water, and pose a risk of transmission. To reduce exposure:
- Avoid drinking untreated water from potentially contaminated sources, such as rivers or ponds.
- Be cautious when swimming in natural water bodies, especially if water quality is a concern.
- Avoid contact with potentially contaminated soil, especially in areas with known animal fecal contamination.
- Follow Guidelines for Pregnant Women: Pregnant women should take extra precautions to prevent coccidian infections, as some parasites can cause complications during pregnancy. This includes following safe food handling practices, avoiding close contact with animals, and practicing good personal hygiene.
- It is important to note that the specific prevention strategies may vary depending on the coccidian parasite in question and the individual’s risk factors. It is advisable to consult with healthcare professionals, veterinarians, or public health authorities for specific guidance and recommendations based on the local epidemiology and individual circumstances.
Keynotes
Here are some key points to note about coccidian parasites:
- Coccidian parasites belong to the phylum Apicomplexa and can infect a wide range of animals, including humans.
- They are microscopic parasites that have complex life cycles, involving both sexual and asexual stages.
- Coccidian parasites are often transmitted through the ingestion of infective stages, such as oocysts, present in contaminated food, water, or soil.
Common coccidian parasites that affect humans include Cryptosporidium spp., Cyclospora cayetanensis, Toxoplasma gondii, Isospora belli, and Sarcocystis spp. - Coccidian infections can cause gastrointestinal symptoms, such as diarrhea, abdominal pain, and nausea, as well as systemic manifestations in some cases.
- Immunocompromised individuals, such as those with HIV/AIDS or organ transplant recipients, are particularly susceptible to severe coccidian infections.
- Laboratory diagnosis of coccidian parasites involves microscopic examination of clinical samples, molecular techniques, immunological tests, and histopathological examination.
- Treatment of coccidian infections typically involves antiparasitic medications, such as nitazoxanide, sulfonamides, pyrimethamine, atovaquone, and clindamycin, depending on the specific parasite and severity of the disease.
- Prevention of coccidian parasites involves practicing good hygiene, ensuring safe food and water, practicing safe animal handling, maintaining clean living environments, implementing food safety practices, being mindful of environmental contamination, and following guidelines for pregnant women.
- It is important to consult healthcare professionals for accurate diagnosis, appropriate treatment, and personalized medical advice regarding coccidian infections.
Further Readings
- “Medical Parasitology” by Markell, Voge, and John.
- “Human Parasitology” by Bogitsh, Carter, and Oeltmann.
- “Tropical Medicine and Parasitology” by Peters and Gilles.
- “Parasitology: A Conceptual Approach” by Perry et al.
- “Foundations of Parasitology” by Roberts and Janovy.
