Staphylococcus haemolyticus- Introduction, Morphology, Pathogenicity, Lab Diagnosis, Treatment, Prevention, and Keynotes
Introduction
Staphylococcus haemolyticus is a bacterium that belongs to the genus Staphylococcus. It is a Gram-positive, coagulase-negative coccus, meaning it has a spherical shape and does not produce the enzyme coagulase, which distinguishes it from its more pathogenic relative, Staphylococcus aureus. Staphylococcus haemolyticus is an opportunistic pathogen, primarily associated with hospital-acquired infections, making it an important focus in healthcare settings.
Here are some key characteristics and information about Staphylococcus haemolyticus:
- Microscopic Appearance: It appears as spherical cells when observed under a microscope. Its cell wall structure contributes to its Gram-positive staining.
- Habitat: This bacterium is commonly found on the human skin and mucous membranes, particularly in the nasal passages. However, it is most notable for its presence in healthcare environments, where it can be a source of nosocomial or healthcare-associated infections.
- Nosocomial Infections: Staphylococcus haemolyticus is notorious for causing infections in hospital settings, including bloodstream infections, urinary tract infections, surgical site infections, and device-associated infections (such as catheter-related bloodstream infections). It often exhibits resistance to multiple antibiotics, making treatment challenging.
- Antibiotic Resistance: Over time, S. haemolyticus has developed resistance to various antibiotics, including methicillin and other beta-lactam antibiotics. This resistance is often attributed to the acquisition of antibiotic resistance genes, which can be transferred between bacteria.
- Coagulase-Negative: Unlike Staphylococcus aureus, which produces coagulase, Staphylococcus haemolyticus lacks this enzyme. Coagulase-negative staphylococci are generally considered less virulent than coagulase-positive ones.
- Biofilm Formation: Staphylococcus haemolyticus is known for its ability to form biofilms on medical devices, such as catheters and prosthetic implants. Biofilms are structured communities of bacteria embedded in a matrix of extracellular polymeric substances, making them more resistant to antibiotics and the immune system.
- Prevention and Control: Preventing Staphylococcus haemolyticus infections in healthcare settings involves strict adherence to infection control measures, including proper hand hygiene, sterilization of medical equipment, and the judicious use of antibiotics to minimize the development of resistance.
- Identification: Identification of Staphylococcus haemolyticus in clinical laboratories is typically done through microbiological cultures, biochemical tests, and molecular techniques like polymerase chain reaction (PCR).
Morphology
The morphology of Staphylococcus haemolyticus refers to its physical characteristics, such as its size, shape, and arrangement. Staphylococcus haemolyticus displays typical characteristics of bacteria in the Staphylococcus genus, which are Gram-positive cocci. Here’s a detailed description of the morphology of Staphylococcus haemolyticus:
- Shape: Staphylococcus haemolyticus is a bacterium with a spherical or cocci (singular: coccus) shape. Cocci are rounded cells, and in the case of Staphylococcus haemolyticus, they are typically arranged in clusters.
- Size: The size of Staphylococcus haemolyticus cocci can vary, but they are generally quite small. Their diameter typically falls within the range of approximately 0.5 to 1.5 micrometers (μm). However, this size can vary depending on growth conditions and other factors.
- Gram Staining: Staphylococcus haemolyticus is Gram-positive. This means that when subjected to the Gram staining technique, its cell wall retains the crystal violet stain, appearing purple-blue under a microscope.
- Arrangement: Staphylococcus haemolyticus cells are often arranged in irregular grape-like clusters, which is a characteristic feature of staphylococci. This clustering of cells is a result of their division in multiple planes, and it gives them their distinctive appearance.
- Cell Wall: Like other Gram-positive bacteria, Staphylococcus haemolyticus has a thick peptidoglycan layer in its cell wall, which contributes to its ability to retain the crystal violet stain during Gram staining.
- Capsule: Some strains of Staphylococcus haemolyticus may produce a slimy, protective capsule around the cell. This capsule can vary in thickness and composition, and it may contribute to the bacterium’s virulence.
- Flagella and Motility: Staphylococcus haemolyticus is generally non-motile, meaning it does not possess flagella (whip-like structures) for movement. It relies on passive dispersion through environmental factors.
- Endospores: Staphylococcus haemolyticus is non-sporulating, which means it does not form endospores, unlike some other bacterial species.
Pathogenicity
Staphylococcus haemolyticus is generally considered an opportunistic pathogen, meaning that it typically causes infections in individuals who are already compromised in some way, such as those with weakened immune systems or who have undergone surgical procedures. While it is not as well-known or as virulent as its close relative Staphylococcus aureus, Staphylococcus haemolyticus can still cause a range of infections. Here are some aspects of its pathogenicity:
- Nosocomial Infections: Staphylococcus haemolyticus is notorious for causing hospital-acquired or nosocomial infections. It is often isolated from patients in healthcare settings, particularly those who have been hospitalized for extended periods, undergone surgeries, or have indwelling medical devices like catheters, prosthetic joints, or central venous catheters.
- Biofilm Formation: One of the key factors contributing to the pathogenicity of Staphylococcus haemolyticus is its ability to form biofilms on medical devices and implantable materials. Biofilms are structured communities of bacteria embedded in a matrix of extracellular substances, making them highly resistant to antibiotics and the host immune response. This ability to form biofilms can lead to persistent infections.
- Antibiotic Resistance: Staphylococcus haemolyticus has demonstrated resistance to multiple antibiotics, including methicillin and other beta-lactam antibiotics. This resistance is often due to the acquisition of antibiotic resistance genes and can complicate treatment.
- Infection Sites: S. haemolyticus can cause a range of infections, including bloodstream infections (bacteremia), urinary tract infections (UTIs), surgical site infections, pneumonia, and skin and soft tissue infections. The specific clinical presentation depends on the site of infection.
- Virulence Factors: While it may not possess as many virulence factors as Staphylococcus aureus, Staphylococcus haemolyticus does produce various enzymes and toxins that can contribute to its pathogenicity. These include hemolysins, proteases, and lipases.
- Immunocompromised Hosts: Infections with S. haemolyticus are often seen in individuals with compromised immune systems, such as patients with HIV/AIDS, cancer, or those on immunosuppressive medications. In these patients, the bacterium may cause severe and potentially life-threatening infections.
- Device-Related Infections: S. haemolyticus is frequently associated with infections related to medical devices, such as catheter-associated urinary tract infections (CAUTIs), central line-associated bloodstream infections (CLABSIs), and infections associated with prosthetic implants.
Lab Diagnosis
The laboratory diagnosis of Staphylococcus haemolyticus involves a series of microbiological tests and procedures designed to identify and confirm the presence of this bacterium in clinical samples. Here are the steps typically involved in the lab diagnosis of S. haemolyticus:
- Sample Collection: The first step is to obtain a clinical specimen from the patient, which may include blood, urine, wound swabs, or other relevant samples, depending on the suspected site of infection.
- Microscopic Examination: A small portion of the clinical specimen is placed on a glass slide and examined under a microscope using Gram staining. S. haemolyticus is Gram-positive and appears as clusters of purple-blue cocci.
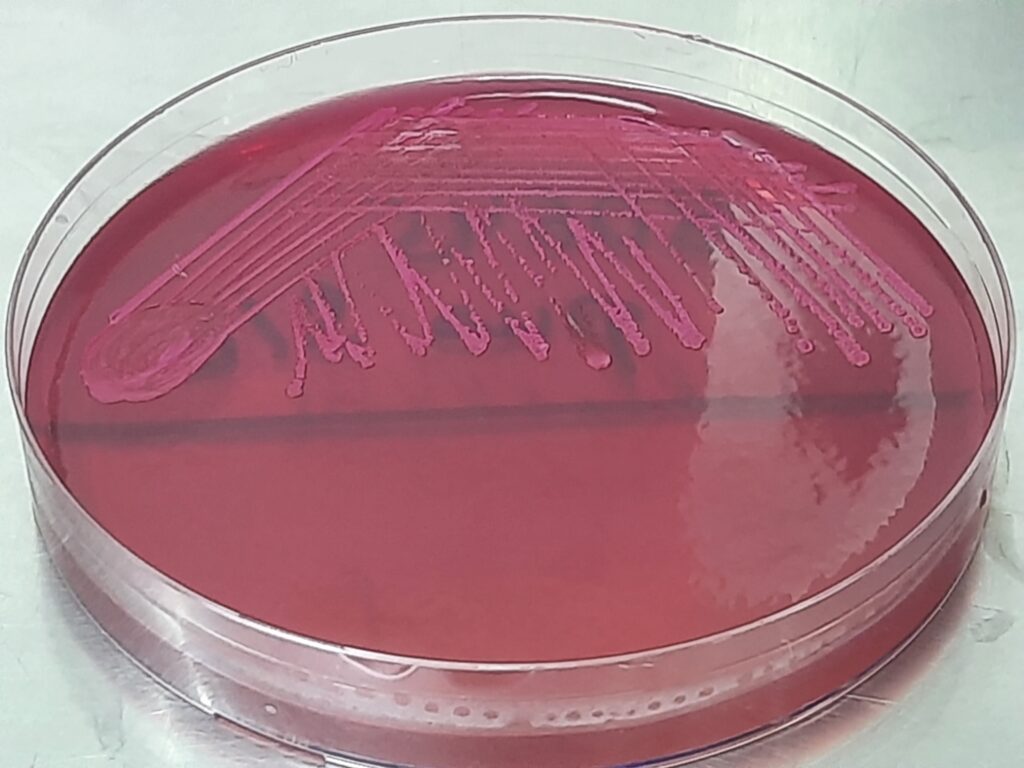
- Culture: The clinical specimen is streaked onto appropriate culture media, such as blood agar or MacConkey agar, and incubated at a suitable temperature (usually around 35-37°C) for 18 to 24 hours. S. haemolyticus typically forms small, circular, raised colonies on solid media.
- Biochemical Tests: After the growth of colonies, various biochemical tests are performed to confirm the identity of the bacterium. Common tests include catalase and coagulase tests. S. haemolyticus is catalase-positive (bubbles when hydrogen peroxide is added) but coagulase-negative.
- Molecular Testing: In some cases, molecular techniques like polymerase chain reaction (PCR) may be used to confirm the identity of the isolate, particularly if precise identification is needed or if antibiotic resistance genes need to be detected.
- Antibiotic Susceptibility Testing: Once the bacterium is identified, antibiotic susceptibility testing is performed to determine which antibiotics are effective against the isolated strain. Given the propensity of S. haemolyticus to develop antibiotic resistance, this step is crucial for guiding appropriate treatment.
- Identification Kits: Commercial identification kits, such as the VITEK system or MALDI-TOF mass spectrometry, may also be used for rapid and accurate identification of S. haemolyticus.
- Biofilm Detection: Given its ability to form biofilms on medical devices, special tests or assays may be employed to detect biofilm production by the isolated strain. These tests can help guide treatment decisions.
- Further Characterization: In certain cases, additional tests may be performed to characterize the strain further, such as determining its genetic profile, identifying virulence factors, or assessing its resistance mechanisms.
It’s important to note that accurate diagnosis of S. haemolyticus is crucial, especially in a healthcare setting, as it can guide appropriate treatment choices and infection control measures. Additionally, antimicrobial susceptibility testing is essential to select the most effective antibiotics, considering the potential for antibiotic resistance in this bacterium.
Treatment
The treatment of infections caused by Staphylococcus haemolyticus can be challenging due to its propensity for antibiotic resistance, particularly to beta-lactam antibiotics like methicillin. Treatment decisions should be guided by the results of antibiotic susceptibility testing, which identifies the specific antibiotics to which the isolated strain is susceptible. Here are some general principles and considerations for the treatment of S. haemolyticus infections:
- Antibiotic Susceptibility Testing: Before starting treatment, it is crucial to perform antibiotic susceptibility testing on the isolated strain. This testing will help identify which antibiotics are effective against the specific S. haemolyticus strain and which ones are not.
- Choice of Antibiotics: The choice of antibiotics should be based on the susceptibility profile of the strain. In many cases, Staphylococcus haemolyticus isolates are resistant to methicillin (MRSH, Methicillin-Resistant S. haemolyticus) and may also exhibit resistance to other antibiotics. Commonly used antibiotics for treatment may include:
- Vancomycin
- Linezolid
- Daptomycin
- Teicoplanin
- Tigecycline
- Clindamycin (if susceptible)
- Combination Therapy: In some cases, combination therapy with two or more antibiotics may be considered, especially for severe or complicated infections. This approach aims to increase the effectiveness of treatment and reduce the risk of resistance development. However, the choice of combination therapy should be made carefully, considering the susceptibility of the strain and potential drug interactions.
- Duration of Treatment: The duration of treatment depends on the type and location of the infection. For bloodstream infections, endocarditis, or other deep-seated infections, treatment may extend for several weeks. Follow-up cultures and clinical assessments are essential to ensure that the infection has been successfully eradicated.
- Biofilm-Related Infections: Staphylococcus haemolyticus is known for its ability to form biofilms on medical devices and prosthetic implants. In such cases, the removal of the infected device may be necessary in addition to antimicrobial therapy. This is often seen with catheter-associated infections and prosthetic joint infections.
- Infection Source Control: Along with antibiotic treatment, it’s important to identify and control the source of the infection. This may involve surgical drainage or debridement of infected tissues and the removal of contaminated medical devices.
- Monitoring and Follow-up: Patients with S. haemolyticus infections should be closely monitored during treatment. Regular assessments of clinical improvement, as well as repeat cultures and susceptibility testing, are essential to ensure the effectiveness of therapy.
- Infection Prevention: Preventing healthcare-associated S. haemolyticus infections is crucial. Infection control measures in healthcare settings, including proper hand hygiene, sterilization of medical equipment, and adherence to infection prevention protocols, can help reduce the spread of this bacterium.
It’s important to note that S. haemolyticus can develop antibiotic resistance, so treatment choices should be made based on the most current susceptibility data. In some cases, consultation with an infectious disease specialist may be necessary to optimize treatment strategies, especially when dealing with complex or refractory infections.
Prevention
Preventing S. haemolyticus infections, especially in healthcare settings, is crucial due to the bacterium’s ability to cause nosocomial or hospital-acquired infections and its propensity for antibiotic resistance. Here are key strategies and measures to prevent the spread of S. haemolyticus:
- Hand Hygiene: Proper hand hygiene is one of the most effective measures to prevent the transmission of Staphylococcus haemolyticus and other healthcare-associated pathogens. Healthcare workers should perform handwashing with soap and water or use alcohol-based hand sanitizers regularly, especially before and after patient contact.
- Infection Control Protocols: Healthcare facilities should have robust infection control protocols in place. These protocols should include guidelines for the proper cleaning and disinfection of surfaces and equipment, as well as the isolation and management of patients with S. haemolyticus infections.
- Catheter Care: To prevent catheter-associated urinary tract infections (CAUTIs), proper catheter care is essential. Catheters should be inserted using aseptic techniques, and their use should be minimized whenever possible. Regular catheter care, including proper cleaning and maintenance, can help reduce the risk of infection.
- Antibiotic Stewardship: Implementing antibiotic stewardship programs is critical in healthcare settings. These programs promote the judicious and responsible use of antibiotics to prevent the development of antibiotic resistance. Avoid using broad-spectrum antibiotics when narrower-spectrum options are effective.
- Patient Screening: Screening patients for S. haemolyticus colonization, especially those at high risk, can help identify carriers and implement appropriate infection control measures.
- Isolation and Cohorting: Patients with known or suspected Staphylococcus haemolyticus infections should be placed in appropriate isolation precautions to prevent the spread of the bacterium to other patients. Cohorting (grouping together) infected or colonized patients can also be considered.
- Medical Device Care: Proper care and maintenance of medical devices, such as central venous catheters and prosthetic implants, are essential to prevent S. haemolyticus biofilm formation. Regular surveillance for device-related infections is important.
- Healthcare Worker Education: Healthcare workers should receive education and training on infection control practices, including hand hygiene, proper use of personal protective equipment (PPE), and the identification and management of S. haemolyticus infections.
- Environmental Hygiene: Routine cleaning and disinfection of healthcare environments, including patient rooms, operating rooms, and common areas, should be performed using effective disinfectants. Pay special attention to high-touch surfaces.
- Surveillance and Reporting: Healthcare facilities should have surveillance systems in place to monitor the incidence of Staphylococcus haemolyticus infections. Prompt reporting of outbreaks or clusters of cases is important for timely intervention and control.
- Vaccination: While there is no specific vaccine for S. haemolyticus, ensuring that healthcare workers and patients receive recommended vaccines, such as the influenza vaccine, can help prevent infections and reduce the overall burden on healthcare systems.
Keynotes
Here are some key points or keynotes on S. haemolyticus:
- Microbial Characteristics: It is a Gram-positive bacterium that appears as spherical cocci, often arranged in clusters. It is coagulase-negative, distinguishing it from its more pathogenic relative, Staphylococcus aureus.
- Hospital-Acquired Infections: S. haemolyticus is primarily associated with hospital-acquired or nosocomial infections, making it a significant concern in healthcare settings.
- Opportunistic Pathogen: It is considered an opportunistic pathogen, typically infecting individuals with compromised immune systems or those who have undergone medical procedures.
- Biofilm Formation: It is known for its ability to form biofilms on medical devices and prosthetic implants. Biofilms contribute to its persistence and resistance to antibiotics.
- Antibiotic Resistance: Many Staphylococcus haemolyticus strains exhibit antibiotic resistance, including resistance to methicillin and other beta-lactam antibiotics. This resistance can complicate treatment.
- Clinical Infections: It can cause a range of infections, including bloodstream infections (bacteremia), urinary tract infections (UTIs), surgical site infections, pneumonia, and skin and soft tissue infections.
- Treatment Challenges: The choice of antibiotics for Staphylococcus haemolyticus infections should be guided by antibiotic susceptibility testing. Vancomycin, linezolid, and daptomycin are commonly used antibiotics when methicillin resistance is present.
- Prevention: Preventing S. haemolyticus infections in healthcare settings involves strict adherence to infection control measures, including proper hand hygiene, sterilization of medical equipment, and antibiotic stewardship.
- Catheter-Associated Infections: Staphylococcus haemolyticus is often associated with catheter-related infections. Proper catheter care and minimization of catheter use are essential for prevention.
- Environmental Hygiene: Routine cleaning and disinfection of healthcare environments are crucial to reduce the risk of transmission.
- Patient Screening: Screening patients, especially those at high risk, for S. haemolyticus colonization can help identify carriers and implement appropriate measures.
- Vaccination: While there is no specific vaccine for this bacterium, vaccination against other infections can help reduce the overall burden on healthcare systems.
- Infection Control Teams: Hospitals should have dedicated infection control teams and protocols to monitor and prevent S. haemolyticus infections.
- Multidisciplinary Approach: Preventing and managing Staphylococcus haemolyticus infections requires a collaborative effort involving healthcare workers, administrators, and infection control specialists.
- Research and Surveillance: Ongoing research and surveillance are necessary to understand the prevalence, antibiotic resistance patterns, and evolving characteristics of Staphylococcus haemolyticus strains.
Further Readings
- Scientific Journals: Consider looking for research articles and reviews in scientific journals related to microbiology, infectious diseases, and clinical microbiology. PubMed, Google Scholar, and journal-specific websites can be valuable resources. Some relevant journals include:
- Journal of Clinical Microbiology
- Clinical Infectious Diseases
- Antimicrobial Agents and Chemotherapy
- Journal of Medical Microbiology
- Microbiology and Immunology
- Textbooks: Textbooks on microbiology, medical microbiology, and infectious diseases can provide in-depth information about Staphylococcus haemolyticus and its related topics. Look for textbooks used in medical or microbiology courses, such as “Murray’s Medical Microbiology” or “Jawetz, Melnick & Adelberg’s Medical Microbiology.”
- Clinical Practice Guidelines: National and international healthcare organizations often publish clinical practice guidelines for the management and prevention of healthcare-associated infections. These guidelines may include recommendations for dealing with Staphylococcus haemolyticus. Check the websites of organizations like the Centers for Disease Control and Prevention (CDC) and the World Health Organization (WHO) for relevant guidelines.
- Review Articles: Review articles provide comprehensive summaries of the current state of knowledge on a specific topic. Search for recent review articles on Staphylococcus haemolyticus in scientific journals or databases.
- Public Health Websites: Government health agencies often provide information on healthcare-associated infections, including Staphylococcus haemolyticus. Visit the websites of agencies like the CDC or the European Centre for Disease Prevention and Control (ECDC) for resources and reports.
- Medical and Microbiology Conferences: Proceedings and abstracts from medical and microbiology conferences can offer insights into the latest research and findings related to Staphylococcus haemolyticus. Look for conference websites and publications.
- Educational Institutions: University and medical school websites may offer educational resources, research papers, and lecture materials related to Staphylococcus haemolyticus.
- Books on Infectious Diseases: Books written by experts in the field of infectious diseases may include sections or chapters dedicated to Staphylococcus haemolyticus and its clinical significance.
- Online Medical Databases: Online databases such as UpToDate and DynaMed provide evidence-based clinical information on a wide range of medical topics, including Staphylococcus haemolyticus.
- Research Centers: Explore websites of research centers and institutes specializing in microbiology, infectious diseases, and antimicrobial resistance. These organizations often publish research findings and reports.
